News from Across Africa: What’s Happening Now
If you want to keep up with current events in Africa, you’ve come to the right place. This page brings you fresh updates and detailed reports on important stories from around the continent. Whether it’s dramatic incidents, court cases, or political moves, we’ve got you covered.
Breaking News Making Waves
Take the recent collapse of a multi-storey building in Nairobi’s Kahawa West. Early Sunday, the building came down unexpectedly, trapping some people under the rubble. Rescue teams jumped into action fast, evacuating nearby areas to stay safe. Officials are still working to figure out how many were inside and how to save them all. This kind of urgent event matters because it affects local communities directly and signals the need for better safety checks.
Legal and Political Stories You Should Know
There’s also drama unfolding in courtrooms. For instance, the Senzo Meyiwa murder trial is attracting attention as the defense challenges cellphone evidence that could change the case’s outcome. Such trials highlight how technology and legal decisions impact justice in Africa. Meanwhile, notable figures like former EFCC Chairman Ibrahim Lamorde have passed, reminding us of the legacy leaders leave behind.
Beyond emergencies and courts, stories about community leaders and social issues also shape our understanding. For example, Governor Adeleke’s call for NYSC members in Osun to promote diversity and integrity shows how leadership influences youth and society.
These updates might seem separate, but they paint a vivid picture of a continent that’s active, diverse, and full of stories affecting millions daily. Bookmark this page to get straightforward news that keeps you in the loop without the fluff. No jargon. Just facts that matter for you and your community.

SASSA Announces October 2025 Grant Payment Dates with R10 Increase
SASSA unveils October 2025 grant dates, giving older persons priority, extending SRD payouts, and adding a R10 uplift across all social grants.

Voddie Baucham Dies at 56: Reformed Pastor’s Sudden Loss Shocks Global Community
Prominent Reformed pastor, author, and educator Voddie Baucham has died at 56 after an emergency medical incident. Serving as president of Founders Seminary in Florida, he previously led African Christian University in Zambia. His historic heart surgeries in 2021 are seen as a possible factor, though the exact cause remains unclear. The Reformed world mourns a scholar, speaker, and family man.

Collapse of Multi-Storey Building in Nairobi's Kahawa West Sparks Urgent Rescue Efforts
A multi-storey building in Kahawa West, Nairobi, collapsed early Sunday morning, leaving several occupants feared trapped under the rubble. Emergency response teams from the Kenya Red Cross and Nairobi County Government are actively working on the ground. Evacuations are ongoing for nearby buildings as a safety precaution. Rescue operations are in full swing, though the number of people inside remains unknown.

In-depth Analysis of BBC's Impactful News Article
This article dissects a BBC News piece, examining the significance and implications of its content. It analyses the newsworthiness, reader reactions, and potential effects on the community and beyond. Additionally, it highlights any new insights gained from the article and possible future developments.

Senzo Meyiwa Murder Trial: Defence Criticizes State's Cellphone Evidence Amid Cross-Examination
During the resumed Senzo Meyiwa murder trial, the defence cross-examined the State's cellphone evidence, illustrating ambiguities between devices and their owners. This argument, exemplified through Longwe Thwala's use of his father's phone, may aid the accused, notably Bongani Ntanzi, whose phone activity conflicted with his police custody. Forensic expert Pinky Vythilingam's testimony is being scrutinized.

Ex-Konga CEO Nick Imudia's Tragic Suicide in Lagos Shocks Community
Nick Imudia, the former CEO of Nigeria's leading e-commerce company, Konga, tragically ended his life on June 25 by jumping off his apartment balcony in Lekki, Lagos. Before his death, he called his brother in the US for wealth distribution instructions and spoke to his young daughter. His untimely death has left friends and family in disbelief, with the motive still unclear.
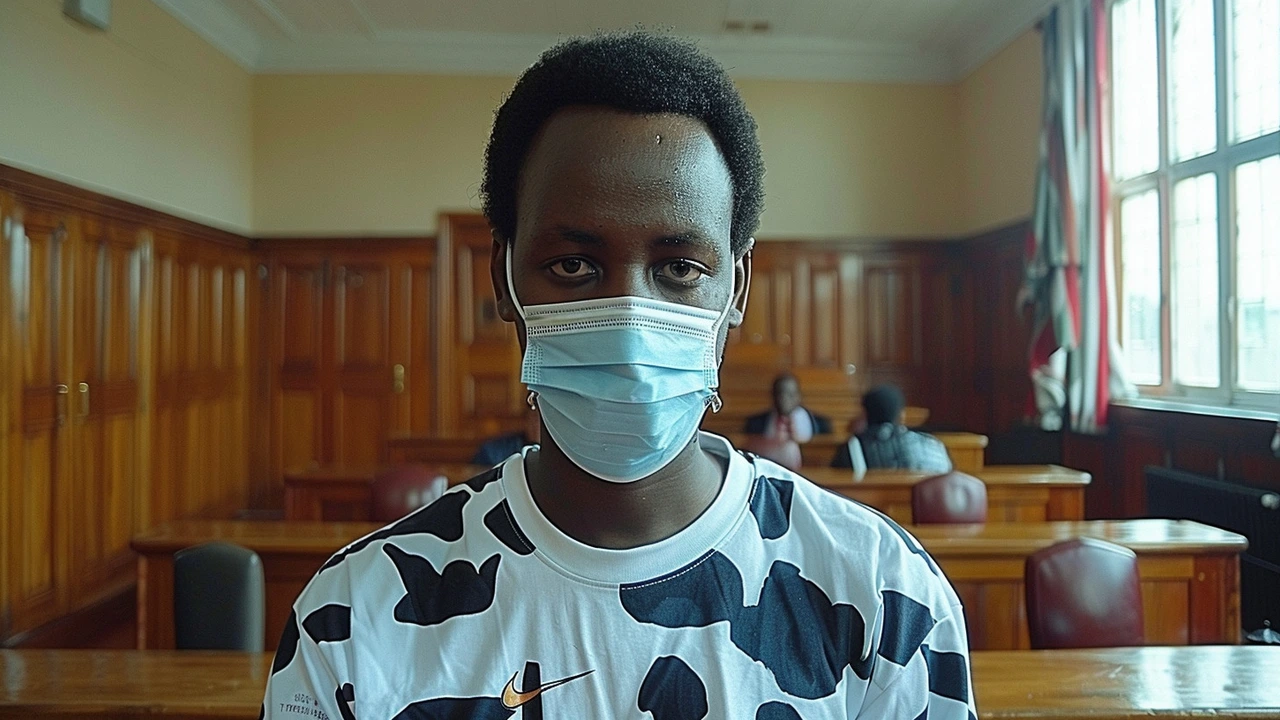
Teen’s Release on Sh700,000 Bond Sparks Debate Amidst Police Assault Allegations
A 19-year-old student, Ian Njoroge, has been released on a Sh700,000 bond by Milimani principal magistrate Ben Mark Ekhubi. Njoroge faces allegations of assaulting a police officer and robbing him of a communication gadget. Despite prosecution objections, the court deemed the charge unconstitutional and rejected claims Njoroge was a flight risk.

Former EFCC Chairman Ibrahim Lamorde Passes Away at 61
Ibrahim Lamorde, ex-chairman of Nigeria's anti-corruption agency EFCC, has died at the age of 61 while receiving medical treatment in Egypt. Lamorde, who joined the Nigerian Police in 1986, rose to Deputy Inspector General of Police and led the EFCC from 2011 to 2015.

Governor Adeleke Encourages NYSC Members in Osun to Champion Diversity and Integrity
Governor Ademola Adeleke of Osun State urges new NYSC members to embody their roles as ambassadors for their communities. He emphasizes embracing diversity, integrity, and making positive impacts during their service year as key success factors.

Enduring Love Amidst Adversity: The Romantic Journey of Michael and Dinah Oyier
Dinah Nasimiyu Oyier, the widow of media personality Michael Oyier, shared their love story at his funeral in Nairobi. She recounted their first meeting during the Covid pandemic, their loving relationship, and the life lessons they shared.
Categories
- Sports (152)
- Politics (24)
- Entertainment (21)
- World (15)
- News (10)
- Lifestyle (8)
- Business (6)
- Technology (3)
- Health (3)
- Environment (2)
Popular Articles



